
Equipping Sierra Leone’s Midwives with Lifesaving Ultrasound Skills
Aminata Sesay lay on the examination bed in Bo Regional and Government Referral Hospital, eight months pregnant with her second child, as a midwife placed a small handheld device against her abdomen. Within moments, an image appeared on the screen. What might have gone unnoticed before became clear. Her amniotic fluid was very low, a condition that can put her baby at risk. With this information, the care team could act quickly and make decisions to protect both mother and child. Aminata was one of several pregnant volunteers who participated in a hands-on training for midwives, to help them strengthen skills that are now improving care for women across the hospital.

Stories like Aminata’s reflect both the progress and the ongoing challenges of maternal care in Sierra Leone. The country has made important gains in reducing maternal deaths, with the maternal mortality ratio declining from 443 to 354 deaths per 100,000 live births between 2020 and 2023. Yet sustaining this progress depends on what happens inside maternity wards every day, where midwives are often the first and most consistent point of care for pregnant women.
At Bo Regional and Government Referral Hospital, which serves around 756,000 people and sees up to 400 pregnant women each month, midwives work in a high-volume environment where timely clinical decisions are critical. For many, assessing pregnancies has long relied on experience and physical examination. As one midwife shared, they depended on measuring tape, fetal dopplers, and palpation to understand a baby’s growth and position. While these methods remain important, they can limit the ability to detect certain complications early.
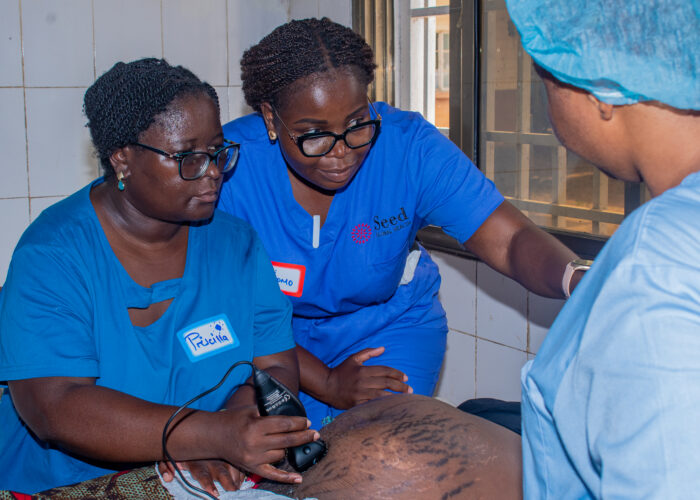
To address this gap, 27 midwife preceptors at the hospital are now being trained in point-of-care ultrasound (POCUS), a simple handheld, rechargeable tool that allows midwives to perform scans directly at the bedside, through a partnership between Seed Global Health (Seed) and the Inteleos Foundation. With five portable devices now available in the maternity unit, midwives can conduct scans during routine visits and emergencies without relying on distant equipment or inconsistent power supply.

The training focuses on practical skills that directly improve care. Midwives are learning how to conduct an overview scan, locate the placenta, assess amniotic fluid, calculate fetal heart rate, and identify multiple pregnancies. These competencies help midwives detect complications earlier, respond more effectively, and guide safer deliveries.
For many of the participating midwives, this marks a shift in their role. Previously, ultrasound was typically performed by doctors or specialized officers, leaving midwives to observe. Now, they are building their confidence and skills to make informed clinical decisions themselves. This shift strengthens not only individual practice, but the entire maternity ward as a place of both service delivery and learning.
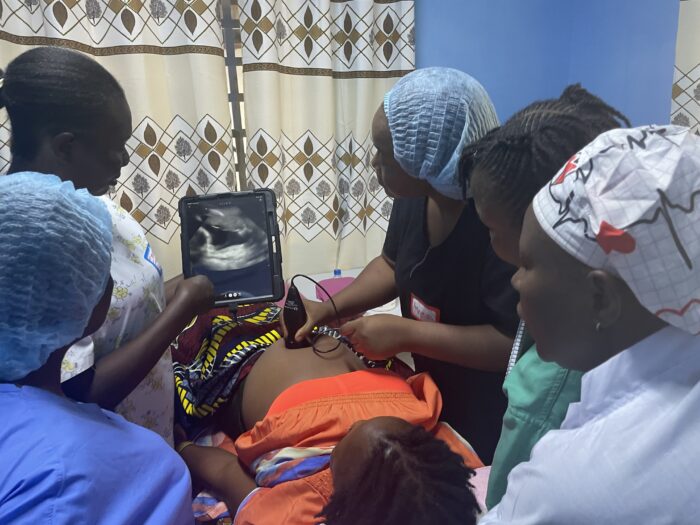
This initiative is part of a broader effort by Seed Global Health to strengthen maternity services in Sierra Leone by investing in midwives as both providers and educators. Through mentorship, preceptorship, and support within clinical environments, midwives are better equipped to deliver high quality care while also training the next generation of midwives. Strengthening these clinical learning spaces improves care today and helps build a more resilient workforce for the future.
The impact is already visible in moments like Aminata’s. When midwives have the tools and training to diagnose more accurately, they can act earlier and with greater confidence. As these skills become embedded in everyday practice, they will help ensure safer pregnancies, better outcomes for newborns, and continued progress in reducing maternal mortality across Sierra Leone.

