Ensuring Access to High-Quality Primary Care
Zambia has made significant improvements in reducing mortality rates related to acute infectious diseases over the last decade. However, the country is experiencing a shifting burden of disease, with a growing prevalence of chronic noncommunicable diseases, that its health workforce is not prepared to address. Shortages of physicians are especially acute in rural areas, where the bulk of Zambia’s populace is concentrated.
In the spring of 2010, a group of educators at the University of Zambia (UNZA) began working to develop a post-graduate training program in family medicine, with the aim of developing physicians who could treat a wide array of medical conditions across the lifespan. The new specialty would be well-suited to administer preventive and curative care in both urban and rural settings.
In the course of three years, Seed Global Health (Seed) engaged in the essential planning and design of the program with the UNZA Family Medicine Working Group and the Ministers of Health and Education. The family medicine MMED program was officially opened in January 2019, accepting its first three registrars. Since then, Seed has provided faculty to offer clinical training through daily teaching rounds at the patient bedside, lectures, simulations, and research mentorship. In addition, Seed has supported curriculum development initiatives and administrative aspects of the program.
My first year has been a great experience. I have enjoyed learning how to carry out procedures that have been known to be outside the scope of medical doctors such as reading ECG and performing ultrasound scans using [point-of-care ultrasound] POCUS. The introduction of POCUS has changed the way I manage patients seen in both outpatient and inpatient settings. The mentorship offered by both senior colleagues and faculty has enabled me to enjoy the training and gain appropriate knowledge to care for patients holistically.
-Dr. Nalukui Wanga, Second Year Registrar, UNZA Family Medicine Residency Program
At the start of 2020, the program established itself at its primary clinical training site—Chilenje Government Hospital in Lusaka. Shortly after, Seed’s two full-time educators arrived. Through our innovative partnership, we have sought to expand the breadth and impact of the program. As such, Seed and UNZA School of Public Health spent the past eight months recruiting and recently held the program’s first ever orientation with seven new residents. We supported a weeklong orientation in January to prepare the registrars for the most common clinical challenges they would face upon entering the wards.
Being able to build a relationship and get to know our patients through continuous lifelong interactions, is a unique feature of family physicians that helps build trust and get to know not only the patient but also treat other family members, regardless of age. During my first year, I am looking forward to learning how to use the POCUS. I am excited to learn how to use this innovative tool that can assist in modifying patient management and will enable us to make potentially life saving decisions right at the bedside. I am also looking forward to learning about standards of care that have been set and being able to adjust and implement them in our low-resource setting in order to improve the quality of care that patients are receiving.
-Dr. Kabanda Mary Musenge, First Year Registrar, UNZA Family Medicine Residency Program
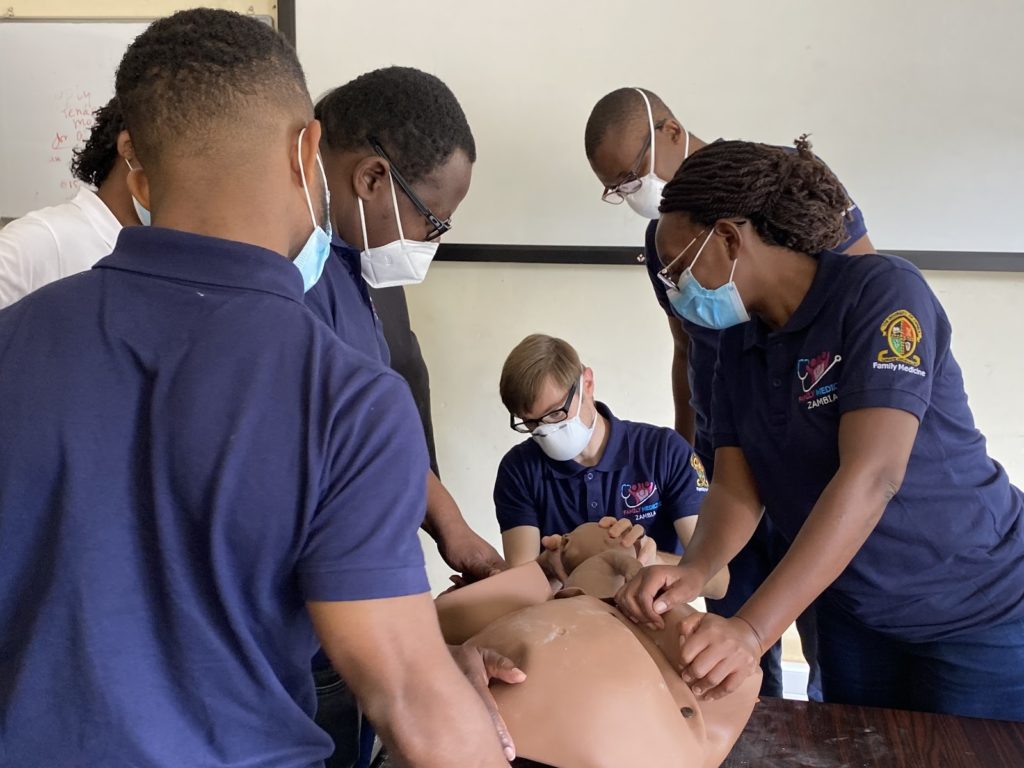
Dr. Haldeman, Seed Educator, demonstrating techniques to resolve complications of labour during a simulation at UNZA, January 2021.
Later this year, Dr. Mpundu Makasa, who was part of the UNZA Family Medicine Working Group, will be the first graduate of the program. She will become a faculty member after graduation, re-investing her newfound skills and experience to teach in the program. We are looking forward to working with Dr. Makasa in her new role as we continue supporting the registrars throughout their four-year program by providing the sustained bedside clinical mentorship that they need.
In a country with very few doctors, adding 10 additional physicians to the front lines of primary care is transformative for communities. The training of family medicine specialists, and placement at the district level hospitals, will allow patients to continuously access quality care closer to their homes and reduce the number of referrals to the provincial and central hospitals. It will also lessen the financial burden and time lost at secondary and tertiary hospitals that are further away from most people’s residences and places of work.
Learn about how we are using POCUS to strengthen primary care in Zambia.


